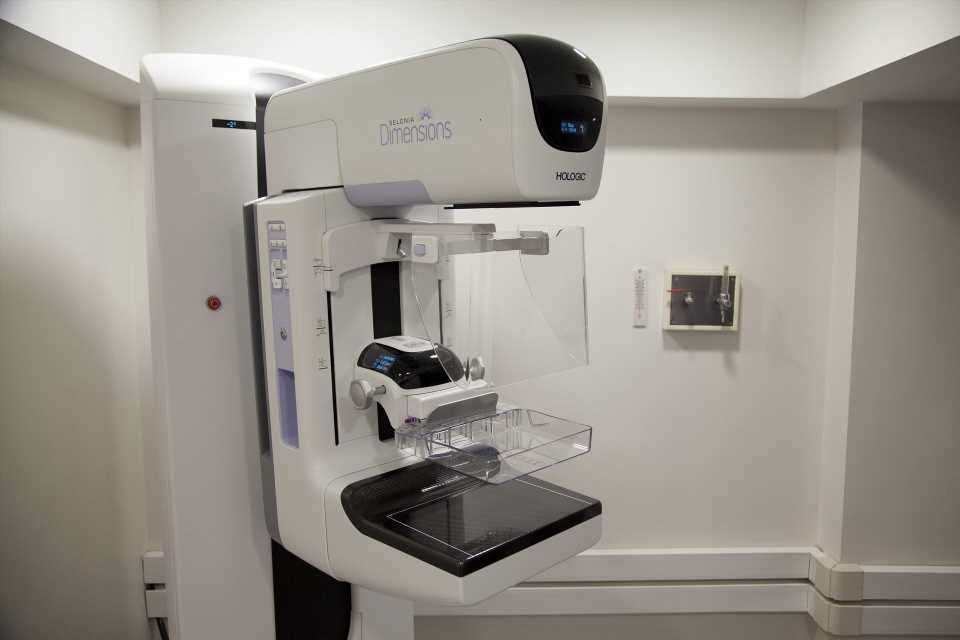
In 2009, the U.S. Preventive Services Task Force changed its mammography screening guidelines to recommend that routine breast cancer screening start at age 50 rather than age 40, recommending an individualized approach for women ages 40-49. The group cited insufficient evidence for screening women ages 75 and older.
Researchers at the University of Vermont Cancer Center, Sarah Nowak, Ph.D., and Brian Sprague, Ph.D., found that the change in guidelines led to a decline in mammography screening rates for all three age groups, including in the 50-74 group most at risk of developing breast cancer and most in need of screenings, an unintended consequence. The researchers coined the the term “spillover” for this effect, since the new guidelines were intended to reduce unnecessary screening for groups less at risk but spilled over to at-risk women.
Their results were recently published in The American Journal of Preventative Medicine.
Data from 2002 through 2018 illustrates that, after 2009, screening rates have fallen nationally by 1.3 percentage points per year for ages 40-49, .5 percentage points per year for women aged 50-74 years old, and 1.7 percentage points per year for 75+.
“While these percentages may seem small, the cumulative impact over 10 years translates to 2.4 million fewer women in the United States aged 50-74 being up to date with screening mammography,” Dr. Sprague said.
The research team is currently exploring why spillover is happening. For example, evidence shows that when women know someone personally diagnosed with breast cancer through screening, they encourage others to get screened. Declining screening for women ages 40-49 and 75+ could lead to women ages 50-74 learning about early-stage breast cancer diagnoses in friends and family less often.
More information:
Sarah A. Nowak et al, Spillover After Mammography Guideline Change: Evidence From State-Level Trends, American Journal of Preventive Medicine (2023). DOI: 10.1016/j.amepre.2023.01.039
Journal information:
American Journal of Preventive Medicine
Source: Read Full Article