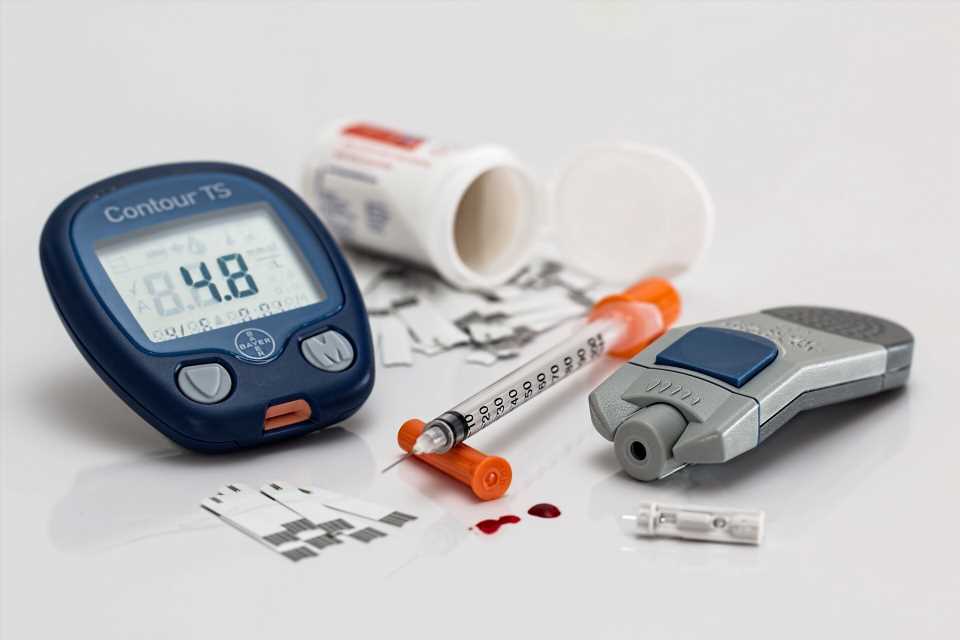
The past few years have seen numerous advances in the understanding of how type 1 diabetes develops and how to manage it, yet the global disease burden remains high, according to a review article published April 5 in The Lancet.
“Our review reveals that despite advances in clinical management, type 1 diabetes remains burdensome and optimal metabolic control is challenging,” says Teresa Quattrin, MD, lead author on The Lancet article, associate dean for research integration in the Jacobs School of Medicine and Biomedical Sciences at the University at Buffalo and UB Distinguished Professor in the Department of Pediatrics.
The authors cite data related to diabetes control in youth and adults from the T1D Exchange demonstrating that only 21% of adults with type 1 diabetes have an A1c (a blood test that reflects a 90-day sugar average) of 7.0 or lower. This is the goal level in order for persons with type 1 diabetes to prevent complications.
While type 1 diabetes is the third most common disease of childhood, there should be greater awareness of adult onset of the disease. The paper references data from the UK Biobank indicating that up to 40% of type 1 diabetes diagnoses occur in people over age 30. Although type 2 diabetes is far more common, with type 1 diabetes accounting for just 10% of total diabetes cases, the paper notes that prevalence of type 1 diabetes is on the rise.
Technologies improve lives of persons with type 1 diabetes
The paper includes a discussion of how increased use of technologies to achieve blood sugar control has proven benefits. Continuous subcutaneous insulin infusion (CSII), also called insulin pump therapy, delivers flexible dosing of fast-acting insulin and can infuse insulin amounts low enough to be suitable for infants and toddlers with the disease.
However, the paper notes that racial and ethnic disparities persist and insulin pump usage is lowest at 18% among non-Latinx Black populations compared with 72% among non-Hispanic white people and 40% among Hispanic populations.
Continuous glucose monitoring, which measures sugar levels in real time without the need for multiple daily finger pricks, can also benefit patients and, when coupled with CSII, can increase blood sugar control and decrease the burden of diabetes management.
The paper also reports that inhaled insulin has demonstrated a fast onset of action, improving the ability to control glucose after meals.
The daily burden of working to achieve blood sugar control results in added mental health challenges, such as anxiety and depression. People with type 1 diabetes are three times more likely to experience depression than people who don’t have the disease. It is therefore recommended that all patients undergo mental health screening.
Obesity is noted as being increasingly present in people with type 1 diabetes, complicating diabetes control and leading to higher rates of associated medical conditions.
“A healthy lifestyle is essential for persons with type 1 diabetes to succeed in pursuing optimal metabolic control, but unfortunately smoking is also observed in persons affected by type 1 diabetes, reflecting the trend in the general population,” says Quattrin.
Preserving and replacing beta cells
Progress is being made in the identification of individuals at higher risk for developing type 1 diabetes; the goal is to treat these individuals with disease-modifying agents in order to preserve pancreatic β-cells, which produce insulin, and delay progression to the stage when they need insulin therapy.
Quattrin adds that the FDA recently approved a medicine called Teplizumab, which delayed the onset of diabetes by about three years in persons at very high risk for type 1 diabetes. The paper notes that another exciting advance in treating type 1 diabetes lies in new, β-cell replacement approaches to treat insulin deficiency, with several treatments now in clinical trials.
“A world without type 1 diabetes seems elusive,” concludes Quattrin, “but advances in disease management and ways to prevent or slow the disease onset are accelerating, giving patients and those of us in the field new hope with exciting opportunities to optimize care for our patients.”
More information:
Teresa Quattrin et al, Type 1 diabetes, The Lancet (2023). DOI: 10.1016/S0140-6736(23)00223-4
Journal information:
The Lancet
Source: Read Full Article