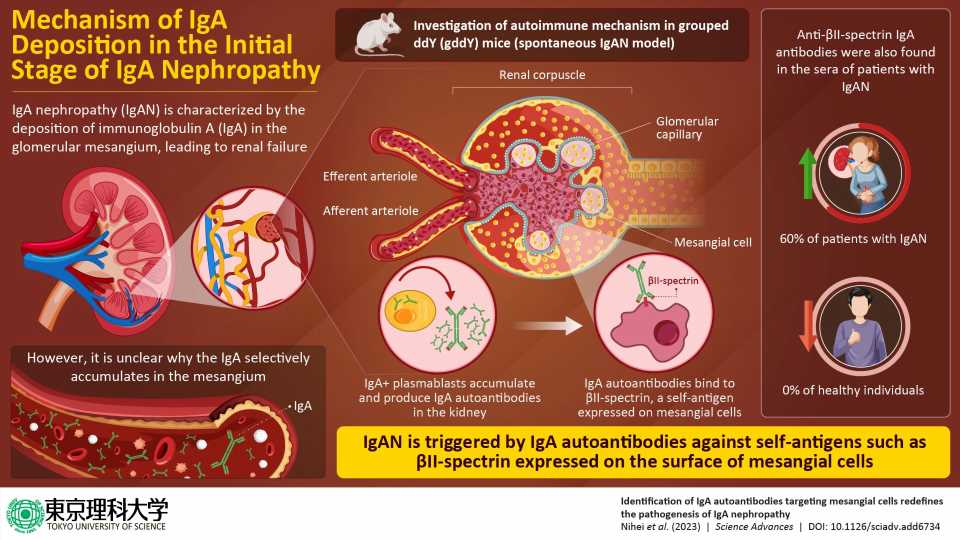
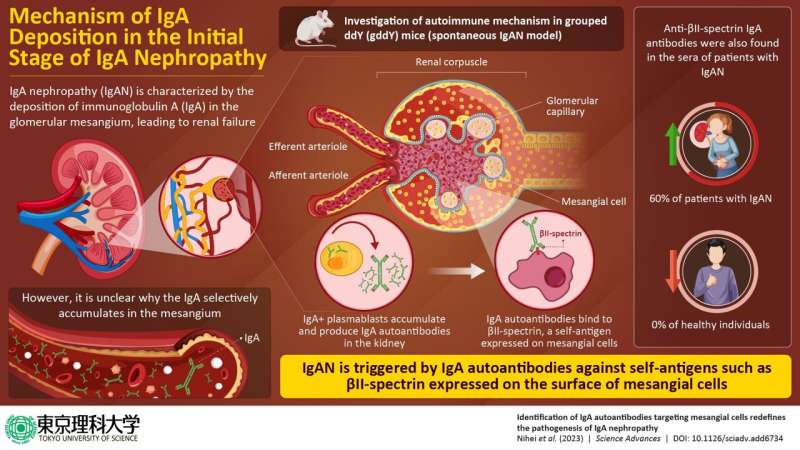
IgA nephropathy (IgAN) is a kidney disorder characterized by the buildup of immunoglobin A (IgA) in the glomeruli, which are bundles of capillaries that filter blood in the kidney. In advanced stages of the disease, the buildup of IgA in the glomeruli disrupts kidney functioning and, in approximately 30% to 40% of cases, leads to kidney failure.
IgA is thought to form complexes with IgG, IgM, and C3 proteins in the blood and then accumulate in the glomeruli during filtration. However, the accepted explanation does not explain a unique hallmark of the disease: during the initial stages of IgAN, IgA deposition is seen in the mesangium, an area composed of mesangial cells and matrix within the glomerulus.
In a study that was recently published in Science Advances, a group of researchers from Japan has uncovered the reason for IgA deposition being restricted to the mesangium. The researchers, including Professor Daisuke Kitamura from Tokyo University of Science and Dr. Yoshihito Nihei and Professor Yusuke Suzuki from Juntendo University, investigated the development of IgAN using specially bred mice, called gddY mice, which exhibit a disease similar to human IgAN.
The researchers found that unlike the serum of control mice that did not develop IgAN, the serum of gddY mice contained autoantibodies (antibodies that attack the cells of one’s own body) that recognize a protein called βII-spectrin found in the mesangial cells. “We have demonstrated that βII-spectrin, previously thought to be an intracellular protein, is in fact exposed on the surface of mesangial cells and directly recognized by the IgA autoantibodies produced by gddY mice. Similarly, anti-βII-spectrin IgA antibodies were found in the sera of many patients with IgAN,” explains lead researcher Prof. Kitamura.
The researchers conducted serum analyses, which revealed that 70% of the gddY mice produced IgA autoantibodies, whereas only 6% of the control mice were found to have them. Similarly, while about 60% of patients with IgAN tested in the study produced autoantibodies to βII-spectrin, none of the individuals in the control group had them. The researchers further discovered that cells producing IgA antibody called IgA+ plasmablasts accumulated in the kidneys of gddY mice and patients with IgAN.
To determine whether IgA autoantibodies specifically recognize and bind to βII-spectrin, the researchers introduced βII-spectrin in embryonic kidney-derived cell line and analyzed by flow cytometry, a laser-mediated analysis of immunofluorescence-stained cells. The result confirmed that the IgA autoantibodies did indeed bind specifically to βII-spectrin on the cell surface. The researchers further confirmed their findings by injecting mice with IgA autoantibodies and visualizing the structures of the glomeruli in kidney using immunofluorescence staining.
“IgA antibodies isolated from gddY mice bound to βII-spectrin on the surface of mesangial cells, and when administered intravenously, bound to the renal mesangial cells. Thus, this study showed for the first time that IgA-type autoantibody production against mesangial cells may be the cause of IgAN,” Prof. Kitamura notes.
Understanding the mechanism of initial disease development in IgAN can help design better treatments for the disease in the future. Moreover, the findings of this study can make testing for IgAN easier than ever before. “Until now, IgAN could only be diagnosed by risky kidney biopsy. Now that we know that 36% to 60% of IgAN patients have IgA-type autoantibodies to beta 2-spectrin in their blood, we will be able to diagnose IgAN using the patient’s blood,” Prof. Kitamura concludes.
More information:
Yoshihito Nihei et al, Identification of IgA autoantibodies targeting mesangial cells redefines the pathogenesis of IgA nephropathy, Science Advances (2023). DOI: 10.1126/sciadv.add6734. www.science.org/doi/10.1126/sciadv.add6734
Journal information:
Science Advances
Source: Read Full Article